Overview of the parasomnias
What are the social and economic costs of
parasomnias?
What are REM sleep parasomnias?
Recurrent isolated sleep paralysis
What are NREM sleep parasomnias?
What other parasomnias are there?
Sleep-related rhythmic movement
disorder
The American Academy of Sleep Medicine defines
parasomnias as “undesirable physical events or experiences that occur
during entry into sleep, within sleep or during arousals from sleep”.1 They are varied in their expression, ranging
from simple movements (rocking, grinding, and groaning) to complex, seemingly purposeful behaviors (sleepwalking,
REM behavior disorder). Most parasomnias are considered to be normal sleep
phenomena and benign, especially when they occur in children. The incidence and
prevalence of these undesirable sleep events decreases significantly with the
onset of adolescence. In some cases they can lead to injuries, psychological
distress and sleep disturbances for both the individual and family members. In
legal cases of sleep-related violence (when a diagnosis of parasomnia has been
established), parasomnias involve behaviors that are not clearly motivated, are
devoid of sound judgment and not under conscious deliberate control.
Parasomnias include many conditions with
different pathophysiologies and responses to treatment. They are currently
classified into primary parasomnias, which are disorders of sleep states per
se, and secondary parasomnias, which are disorders of specific organ systems
that manifest preferentially during sleep.
Primary parasomnias are further classified into 1) disorders associated
with NREM [non-REM] sleep (aka disorders
of arousal), 2) parasomnias associated with REM sleep and 3) other
parasomnias. Each of these divisions is further subdivided into more specific
parasomnia types; subdivisions for the primary parasomnias are shown in Table
1.
Table
1. Primary parasomnias classified by sleep stage
|
Parasomnias associated with
NREM sleep |
Parasomnias associated with REM
sleep |
Other parasomnias |
|
|
|
|
|
|
|
What are the social and economic costs of parasomnias?
Sleep is central to good health and daily functioning. Yet the full scale of the social and economic costs incurred by sleep disorders is not yet completely clear. For 2004, the direct and indirect cost of sleep disorders as a whole was estimated to be $7.5 billion for the Australian population (20.1 million people). This would translate to about $109 billion for the United States2 and $12.3 billion for Canada. But little is known about the economic impact of specific parasomnias. At least two parasomnias, sleepwalking and RBD, warrant more immediate attention because of the injuries and severe sleep disruption they often inflict on patients and their families.
Adult sleepwalking can lead to the destruction of property such as the breaking of walls, doors, windows and plumbing. Behaviors reported for either somnambulism or sleep terrors include running into walls and furniture, jumping out of windows, driving a car, wandering around streets, climbing ladders, sexual activity and manipulating weapons—even loaded shotguns. The fact that somnambulistic episodes can consist of complex and organized behaviors such as suspected suicide, attempted homicide and homicide, raises important medico-forensic questions.3-12 The number of legal cases of sleep-related violence is on the rise13.
RBD can frequently lead to serious injuries 14,15 and are a main reason for clinical
consultation. RBD episodes may also cause severe sleep disruption for the bed
partner and major marital discord, mood changes, even suicide attempts.16 Beyond these consequences, RBD may be a prodrome for neurodegenerative diseases, especially Parkinson
and Lewy body diseases. In fact, 45% of patients
with RBD develop either Parkinson disease, Lewy body disease or multisystemic
atrophy after a follow-up of only 5 years.17 A longer follow-up (11 years) reveals that 65%
of RBD patients develop a neurodegenerative disorder leading mainly to
dementia.18
What
are REM sleep parasomnias?
Clinical features
Nightmare disorder is the persistence of
disturbing dreams that arise primarily from REM sleep (more rarely from stage 2
sleep) and that usually end up awakening the sleeper.1 Autonomic activation is usually much less than
in sleep terrors. There may be dream-enacting behaviors at the end of some nightmares, especially if
you are enduring a situation of intense emotional stress and/or sleep
disruption, e.g., the postpartum state.19 Awakenings from nightmares are usually abrupt
and a detailed disturbing dream is easily recalled. Idiopathic nightmares have no apparent cause and are distinguished
from post-traumatic nightmares, which
are due to trauma.
Incidence and prevalence
The prevalence of nightmare symptoms is
estimated together with their frequency. Nightmares occur occasionally in over
85% of the general population, at least once a month in 8-29% and at least once
a week in 2-6%.20-23 A frequency of one nightmare per week likely
reflects clinical pathology. Nightmares are less frequent among preschoolers
(1.5-3.9% parents report their children have them often or always) than
previously thought but may appear as early as 29 months and remain highly
stable until age 6 yrs.24 An internet survey of 24,102 respondents25 found the number of nightmares recalled per month
peaks between ages 20-29 and then declines steadily. A second internet survey
of 3978 respondents found that the distress caused by nightmares increased
abruptly at an earlier age for women than for men. A gender difference favoring
girls appears in adolescence26,27 and continues throughout the lifespan, as
shown in Figure1.25
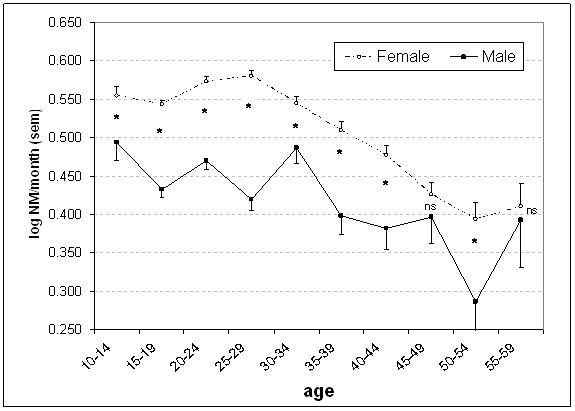
Figure 1.
Retrospective
estimates of monthly nightmare frequency by 5-year age strata in an internet
sample of 24,000 respondents.25
*=significant difference between female and male subjects at that stratum,
p<.05
Polysomnographic characteristics
Nightmares are often associated with autonomic
fluctuations (increased heart and respiratory variability) during REM sleep.
But these fluctuations are often less than might be expected from hearing the
content of the nightmare.28 In contrast, post-traumatic nightmares are
accompanied by heightened reactivity in the form of more frequent awakenings,29 longer time awake after sleep onset,29,30 increased motor and rapid eye movement
activity during REM sleep,31-33 and higher REM and NREM sleep respiration
rates.34 Both idiopathic and post-traumatic nightmare
patients have elevated levels of periodic leg movements (PLMs) in REM and NREM
sleep.29
Associated factors
A genetic contribution to nightmares has been found to be 44% for men and 45% for women in the case of childhood nightmares.35 Bad dreams among 29-month-old preschoolers are predicted by mother ratings of difficult temperament as early as 5 months of age and by mother and father ratings of child anxiety as early as 17 months.24 Among adults, nightmares are also associated with psychopathological traits36,37 and personality variables such as:
* physical and emotional reactivity36,38
* fantasy proneness39
* thin boundaries.40-43
Nightmares are more frequent and prevalent in
psychiatric populations23,44 and are associated with pathological symptoms
such as anxiety, neuroticism, posttraumatic stress disorder,
schizophrenia-spectrum symptoms, suicide risk, dissociative phenomena,
problematic health behaviors and sleep disorders (see reviews45,46). Nightmares are also more likely during
periods of increased life stress.38,47,48
Recurrent isolated sleep paralysis
Clinical features
Recurrent isolated sleep paralysis (aka
isolated sleep paralysis or sleep paralysis, SP) is common and generally
benign, being characterized by brief episodes of motor or vocal paralysis combined
with a waking state of consciousness.1 Frightening dreamlike hallucinations often
intrude and can cause considerable distress. SP episodes occur at sleep onset
(hypnagogic) and upon awakening (hypnopompic) and is one characteristic of individuals
with narcolepsy, which is characterized by cataplexy and excessive daytime
sleepiness in addition to SP and hypnagogic hallucinations.1 SP is commonly associated with feelings of
fear or terror49 and are often linked to the hallucination of
an unseen presence in the room (‘sensed presence’).50,51
Incidence and prevalence
Variations in prevalence estimates (5-40%)
depend upon differences in operational definitions, age of subjects and
sociocultural factors.52-54 Age of onset is typically 14-17 yrs.
Accompanying sensed presence hallucinations occur in 60-69% of cases.50,51,55,56
Polysomnographic characteristics
SP episodes most often arise from sleep-onset
REM periods (see Figure 2),57,58 leading to the view that the episodes are bouts
of state dissociation during which some REM sleep mechanisms–muscle
atonia and vivid dreaming in particular–intrude upon the waking state.59,60
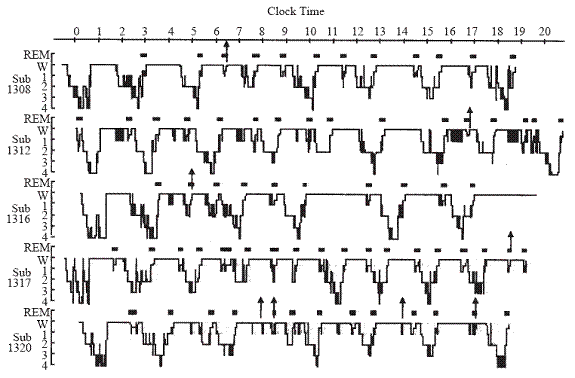
Figure 2.
Somnograms
of five healthy subjects reporting sleep paralysis episodes during a
multiphasic sleep-wake schedule. Vertical arrows above somnograms indicate
awakening points where sleep paralysis episodes were reported. Of 184
awakenings, 8 sleep paralysis episodes were recorded; 2 just prior to impending
REM episodes (spontaneous awakenings) and 6 from sleep onset REM episodes (from
Takeuchi, et al., 2002).58
Associated factors
Among the factors associated with sleep
paralysis episodes are stress,54,58,61 shift work and irregular sleep-wake schedules.53,61 A genetic component has also been reported,
e.g., 36% of respondents in a Japanese sample had family members who
experienced sleep paralysis.62
Several studies link sleep paralysis to various
neurological and psychiatric disorders. It is predicted by bipolar disorder,
automatic behavior and use of anxiolytic medications.52 It is also comorbid with PTSD,63,64 depression symptoms,65,66 anxiety disorder with agoraphobia,67 panic disorder,64,68,69 generalized anxiety disorder and social
anxiety.70 This wide comorbidity has recently been
attributed to mediation by an affect distress personality style (‘sleep
paralysis distress’) in a manner analogous to that proposed for nightmare
disorder (‘nightmare distress’).50
Associations of SP with psychiatric conditions
vary among ethnic groups. Atypically high rates were found in African Americans
with panic disorders,69 Moroccan patients,71 Magrebins71 and Cambodians.63 Some of these differences may stem from cultural interpretations of
sleep paralysis hallucinations, sensed presence in particular, as a form of
spiritual entity, e.g., “ghost
oppression” in China,61 “Old Hag” in Newfoundland,72 “the ghost that pushes you down” in Cambodia,63 among many others.
Clinical features
REM sleep behavior disorder (RBD), first
described as a clinical entity in 1986,73 is characterized by the loss of skeletal
muscle atonia normally present during REM sleep and the occurrence of complex
dream-enacting motor behaviors. Diagnostic criteria include a) complaint of
violent or injurious behaviors during sleep, b) limb or body movements
associated with dream mentation and c) one of the following:
* harmful or potentially harmful sleep behaviors
* dream appears to be acted out
* sleep behaviors disrupt sleep continuity.
In addition, the dream process and its content
appear altered. Most patients (87%) report that their dreams become more vivid,
intense, action-filled, and violent with the onset of RBD.74 Dream themes associated with behaviors are
largely stereotyped in structure and emotional content.73,75 Among published reports of dreams for which
investigators identified specific behaviors, the most frequent pattern is of
vigorous defense against attacks by people (58.8%) and animals (23.5%) (see
review76). Analyses of recently remembered dreams
reveal a high percentage of aggressive contents but, paradoxically, normal
levels of aggressiveness during the daytime.77
Sleep behaviors can produce injuries to the
patient or the bedpartner; these might include ecchymoses, lacerations,
fractures and subdural hematomas. Injuries are a main reason for consultation,
being reported by 79%-96% of consulting cases.14,15
Incidence and prevalence
The prevalence of RBD is still largely unknown.
A telephone survey of violent and injurious sleep behaviors in the British
general population (N=4972; 15-100 yrs of age) produced a prevalence of about
0.5 %.78 Another study of 1034 Hong Kong area residents
(70+ yrs) found a prevalence of 0.4%.79 It is predominant in males (87%), primarily
men over age 50.74 Milder forms of RBD with less aggressive
behaviors that do not lead to clinical consultation have been postulated for
women.74 Also, dream-enacting behaviors among healthy
young students and pregnant and postpartum women have recently been identified
by our group.19,80
Polysomnographic characteristics
Laboratory recordings reveal intermittent or complete loss of REM sleep muscle atonia and excessive phasic EMG activity during REM sleep.75 The PSG diagnostic criteria are presence of:
a) excessive augmentation of chin EMG tone
b) excessive chin or limb phasic EMG twitching
c) one of the following features during REM sleep:
* excessive limb or body jerking,
* complex, vigorous or violent behaviours
* absence of epileptic activity.
Compared with age-matched controls, RBD
patients have more SWS81 and distinct changes in the EEG spectrum
(e.g., more NREM delta,81 less REM occipital beta,82 more theta in several areas).
Associated factors
RBD is strongly associated with
neurodegenerative diseases, especially the synucleinopathy type83 which include:
* Parkinson’s disease,84,85
* dementia with Lewy bodies,86-88
* multiple system atrophy.89-91
RBD is also comorbid with two tauopathies: Alzheimer’s disease92 and progressive supranuclear palsy.93
Even patients with idiopathic RBD show some
signs of neurodegeneration. FDG-PET brain imaging of cognitively normal
patients with dream-enacting behaviors revealed lower metabolic activity in
several brain regions known to be affected in dementia with Lewy bodies.94
Multiple dysfunctions for RBD patients have
been described, including:
* olfactory deficits95
* color identification deficits95
* decreased motor speed95
* EEG slowing,82
* mild dysautonomia96,97
* subtle neuropsychological dysfunctions.82,98,99
RBD has also been associated with narcolepsy and other neurological
disorders,75 such as:
* olivopontocerebellar degeneration
* ischemic cerebrovascular disease
* multiple sclerosis
* Guillain-Barré syndrome
* Shy-Drager syndrome
* Arnold-Chiari syndrome.
What are NREM sleep parasomnias?
Clinical features
Confusional arousals (aka sleep drunkenness)
are transitory states of confusional behavior or thought occurring during or
after awakenings from NREM sleep, usually from NREM sleep early in the night.
The individual is confused, disoriented, behaviorally slow, and may display
automatic or inappropriate behaviors. Vivid dreaming is usually not present.
Sleep-related abnormal sexual behaviors, such as masturbation, sexual
molestation, initiation of sexual intercourse and loud sexual vocalizations
during sleep are part of the spectrum of confusional arousals.1
Incidence and prevalence
The incidence is unknown but episodes are
frequent in early childhood and diminish after age 5.100 Young children with persisting confusional
arousals often become sleepwalkers in adolescence. Prevalence in adults is 3-4
%101. There is no known gender difference.
Polysomnographic characteristics
The arousals usually occur during the first two
NREM episodes, but can also occur in later NREM sleep. PSG recordings have
shown awakenings from NREM sleep.
Associated factors
Childhood confusional arousals are usually
benign; in adults they are often associated with mental disorders or
obstructive sleep apnea. They occur more often in night-shift or rotating-shift
workers.101 Many conditions can set the stage for
confusional arousals:
* family history
* sleep deprivation
* obstructive sleep apnea
* drug/alcohol use.
Clinical features
Sleepwalking is characterized by behaviors
usually initiated during arousals from NREM sleep; it may begin with simple
movements, such as sitting up in bed, and culminate in walking, running out of
the room,1 or, more rarely, more complex activities,
e.g., cooking or eating,102 driving,11 even homicide.3,103-106 Episodes are accompanied variously by amnesia,
confusion, perceived threat, dreaming or even pseudo-hallucination. Usually
considered benign in children, sleepwalking in adults may lead to injuries.
Incidence and prevalence
Peak incidence (approximately 17%) is around
age 12 years.107 For adults, a suggested prevalence of 2-2.5%21,52 is probably an underestimate. Many studies
report no gender difference in older children, adolescents or adults,107,108 but studies of young children 2.5-6 and 4-9
years old found it to be more common in boys than in girls.109,110
Polysomnographic characteristics
Sleep architecture does
not differ between adult somnambulistic patients and control subjects,111-116 except that somnambulists have more arousals out of NREM sleep.111,113 Episodes of somnambulism
are rare in the sleep laboratory, but they may be triggered experimentally by
extended sleep deprivation (e.g., 38 hours).117,118
Associated factors
There is a strong genetic component119 with a link to the HLA-DQB1 gene.120 Anxiety may increase occurrences.100,121,122
Clinical features
Sleep terrors (aka night terrors or pavor
nocturnus) are “arousals from SWS accompanied by a cry or piercing scream
and autonomic nervous system and behavioral manifestations of intense
fear”.1 Typically, within 90 minutes of
falling asleep, the individual screams and sits up with a panic-stricken
expression and intense autonomic activity (sweating, racing heart, rapid
breathing). Less often there are complex behaviors such as leaving the bed,
fleeing the room or thrashing around. Injuries may result in such cases.123 Inconsolability is a key feature; attempts to
console or awaken a somnambulist in mid-episode may well prolong or intensify
it—even causing aggressive actions toward the intervener. As is the case
for somnambulism and confusional arousals, the individual usually does not wake
up fully from a sleep terror and will forget the event the following day. Sleep
terrors do not differ markedly from somnambulism except that the behaviors displayed
are usually more rapid and abrupt than during somnambulism.
Incidence and prevalence
Reported incidence estimates are variable.108,124-126 Some parents may fail to differentiate
nightmares and sleep terrors but when a clear definition is supplied, a high
prevalence (40%) is seen in preschoolers.110 Sleep terrors tend to resolve in adolescence
and do not display a gender difference.108,110 In adults, there is a high degree of overlap
among confusional arousals, somnambulism and sleep terrors.
Polysomnographic characteristics
Sleep recordings often show sudden awakenings
from NREM sleep, especially in the second half of either of the first two NREM
sleep episodes. The amount of time spent in stages 3 and 4 NREM sleep prior to
an episode is positively correlated with severity of the subsequent episode.123 Rarely, they may occur in NREM stage 2.
Associated factors
Childhood sleep terrors are usually not
associated with a neurological condition, whereas onset in adulthood may be. As
is the case for somnambulism and confusional arousals, genetic factors play a
major role. Monozygotic twins are
more concordant than dizygotic twins for sleep terrors127 and they are twice as frequent in children for
whom one or both parents have a sleepwalking history than for those with
non-affected parents.128
What other parasomnias are there?
Clinical features
Sleep enuresis is characterized by recurrent
involuntary voiding during sleep at least twice a week among individuals who
are at least five years of age.1 It is considered primary if the child has
never been constantly dry during sleep and secondary when the child (or adult)
had been previously dry for at least six consecutive months and started wetting
at least twice a week for at least 3 months.
Incidence and prevalence
Three population-based studies110,129,130 found that between 20 and 33% of
children were bedwetting at the age of 5 years. A male predominance in
prevalence is well-established.108,110,129,130 Adult enuresis is rare, occurring in about 3%
of elderly women (65+ yrs) and 1% of elderly men living at home.131
Polysomnographic characteristics
Although parents commonly consider sleep
enuresis to be caused by sleeping too deeply, consistent changes in sleep depth
and sleep architecture have not been demonstrated.132 However, a study using polysomnographic
recording has shown that enuretic boys are more difficult to arouse from sleep
than are age-matched controls.133 For most children, micturition occurs in the
first half of the night and is not associated with a specific sleep stage.132 Tachycardia and short EEG arousals are often
seen prior to enuretic events.132
Associated factors
An association
between enuresis and delayed achievement of early childhood developmental
milestones such as motor skills (for boys) and language (for girls) has been
demonstrated.134 This indicates that bed-wetting may reflect
delayed development of the central nervous system. Enuresis is not linked with anxiety in
preschoolers110 but is in older children.135-137 However, anxiety is more likely a
consequence than a cause of enuresis. Hereditary factors have been recognized;
it is inherited via an autosomal dominant
mode of transmission.138
Prevalence is 77% when both parents were enuretic as children and 44% when one
parent was enuretic.139
Clinical features
Sleep related bruxism is the grinding or
clenching of one’s teeth during sleep, usually in association with sleep
arousals.1 This activity results in tooth wear,
headaches, jaw dysfunction and pain. Orofacial morphology is not likely a
causal factor since it has been shown not to differentiate sleep bruxers from
controls.140
Incidence and prevalence
Sleep bruxism is very common in early
childhood. A recent longitudinal, population-based study found that the
prevalence increases from 2.5 yrs to reach 33% at 6 yrs of age.110 Another longitudinal study reported a
progressive decrease toward adolescence attaining 9% at age 13.108 An age-related decline in prevalence has also
been described throughout adulthood in a population-based study.141 Overall prevalence in adults has
been estimated to be around 8%.142 No gender difference has been found for either
children108 or adults.141 The presence of sleep bruxism in childhood and
adulthood are highly correlated.143
Polysomnographic
characteristics
Although abnormal tooth wear is highly
indicative of sleep bruxism, a definite diagnosis rests on the presence of
rhythmic masticatory muscle activity and grinding sounds during all-night
polysomnographic recording. Bruxism episodes most frequently occur in stages 1
and 2 but can occur in all stages.144,145 Bruxers have normal sleep architecture and
high sleep efficiency, i.e., greater than 90%.144 However, a clear sequence of cortical to
cardiac activation preceding jaw motor activity in bruxism patients146 suggests that sleep bruxism is secondary to
micro-arousals. In fact, both micro arousals and rhythmic masticatory muscle
activity/sleep bruxism episodes were to shown to increase prior to each REM
sleep period (see Figure 4).147
Associated factors
Anxiety has been reported as an associated
factor in children,108 adolescents and adults.148,149
Smoking also exacerbates bruxism.150 As is the case for many parasomnias, there is
a strong genetic influence.143
Sleep-related rhythmic movement disorder
Clinical features
Sleep-related rhythmic movement disorder is
characterized by the repetitive, stereotyped, and rhythmic activity of large
muscle groups that occurs predominantly during drowsiness (sleep onset) or
sleep.1 It can involve any body part although the most
frequent rhythmic movements are body rocking, head rolling and head banging.
Body rocking may be difficult to distinguish from head banging because the
latter movement sometimes includes banging of the head into a solid object. It
is largely a parasomnia of infancy and early childhood. The frequency of
movements ranges between 0.5 and 2.0 Hz but are more typically around 1 Hz.151
Time spent in rhythmic motion can vary from a few seconds to more than
an hour151 but in most cases will occur nightly or almost
every night.152 The majority of episodes (around 80%), at
least for head banging, occur at sleep onset.152 When appearing at sleep onset, rhythmic
movements are considered to be self-soothing or tension-releasing behaviors
linked with pleasurable sensations that have hypnotic properties. However, more
violent movements, usually in cases of mental retardation, can cause eye or
head injuries.153-155
Incidence and prevalence
In infancy, this parasomnia is quite common but
decreases rapidly in prevalence with increasing age. Incidences of 66% at 9 mo, 26% at 2 yrs and 6% at 5
yrs had been reported using a sample of children156 but a recent epidemiological study reported
lower incidences of about 6% at 2.5 yrs, 3% at 4 and 5 yrs and 2% at 6 yrs.110 Body rocking was found present in 3% of
children aged 11 to 13 yrs.108 In rare cases, rhythmic movement disorder
persists into adulthood. No gender differences have been demonstrated.
Polysomnographic characteristics
Different case reports indicate that rhythmic
movement disorder can arise from REM sleep, NREM sleep or sleep onset with
persisting activity in light sleep. Longer movements are usually observed at
sleep onset and during stage 1 sleep whereas shorter movements are seen in
stages 2, 3, 4 and REM sleep.151 Sleep-related rhythmic movements are not
preceded by EEG changes as are nocturnal seizures151 and do not provoke arousals or interrupt SWS
even in older children.152,157
Associated factors
There are no reports of rhythmic movement
disorder in association with other parasomnias or sleep problems except for
restless legs syndrome, which is associated with body rocking.158 Cases of adult rhythmic movement disorder are
not usually associated with severe psychiatric disorders as previously
believed. However, some studies have reported daytime complaints such as
attentional difficulties, sleepiness, morning headaches, fatigue and poor
concentration, and even more serious problems such as anxiety, depression,
hyperactivity and irritability.151,159,160 Whether the daytime symptoms result from poor
sleep caused by the rhythmic movements remains to be determined.
Clinical features
Somniloquy, also known as sleep talking, is
defined as talking during sleep “with varying degrees of
comprehensibility”.1 Somniloquy is such a prevalent phenomenon that
it is considered to be a normal sleep behavior, especially in childhood.
Incidence and prevalence
Although considered the most frequent
parasomnia, somniloquy is usually without consequences and thus rarely a reason
for consultation. Its prevalence among preschoolers (84%110) is much higher than among older children and
adolescents. A prevalence of 30% was found for children aged 11 to 13 yrs using
mainly retrospective reports108 while in adults, an estimate of 24% was found
using a telephone sampling method.78 There is no apparent gender difference.
Polysomnographic characteristics
Somniloquy can arise from all sleep stages.161 Since there are few systematic
polysomnographic studies, no clear profiles have been identified. However,
EMG-induced artifact is common and may begin several seconds prior to, and
continue for several seconds after, verbalizations.162 Temporary suspension of eye movements and the
occurrence of sustained alpha EEG trains during REM sleep somniloquy episodes
have also been noted162 as has suppression of theta and alpha activity
prior to the utterances.163 Episodes frequently occur in parallel with
sleep mentation, but concordance between verbal utterances and ongoing dreamed
speech may vary from isomorphic to completely absent.164 As shown in Figure 3, concordances of any kind
are more common in REM (82.6%) than in stage 2 (58.2%) or stage 3-4 (34.4.1%)
sleep.162
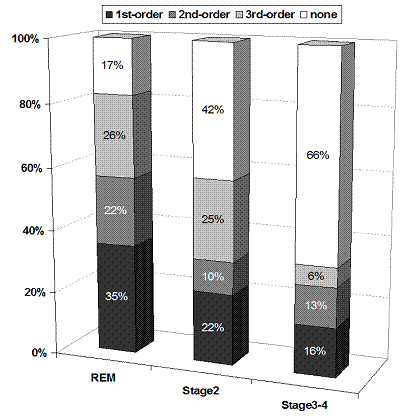
Figure 3.
Sleep-speech
/ mentation-report concordances in relation to sleep stage (N=122 samples). All
3 types of concordance are more frequent for reports from REM sleep (82.6%)
than for reports from Stage 2 (58.2%) or Stage 3-4 (34.4%) sleep (N=23, 67, 32
reports respectively; awakenings with no recall were not included). 1st-order
concordances: same words were both spoken and dreamed; 2nd-order concordances:
conceptually related words were spoken and dreamed; 3rd-order concordances:
dreamed words referred only nonspecifically to spoken words (adapted from
Arkin, 1981, p. 120, Table 7.6).162
Associated factors
Since somniloquy is so prevalent, it is
virtually impossible to isolate predisposing factors. Nonetheless, there is a
clear genetic influence.165 Somniloquy is also the parasomnia that most
often co-occurs with other parasomnias. It often accompanies the behavioral manifestations
of either REM sleep behavior disorder or somnambulism. Stereotyped
vocalizations can also be heard during nocturnal seizures. In most cases,
however, somniloquy is idiopathic.
Clinical features
Also known as catathrenia, sleep-related
groaning is defined as “a chronic, usually nightly, disorder
characterized by expiratory groaning during sleep, particularly during the
second half of the night”.1 Groaning or moaning sounds typically begin two
to six hours after sleep onset. The sounds produced are usually loud but the
pitch and timbre vary among individuals: groaning, loud humming, roaring, and
high-pitched sounds have all been observed. By contrast, within individuals the
type of sound is usually fairly constant. Catathrenia is not associated with
abnormal motor activity and is qualitatively different from somniloquy. Degree
of concordance with sleep mentation is unknown. The affected individual is
usually unaware of the problem and, apart from occasional complaints of daytime
sleepiness, typically has no other sleep complaints. However, production of the
sounds may disturb the bed partner. The identification of this disorder is
relatively new, with approximately
45 cases in total reported in the literature.166-176
Incidence and prevalence
Nocturnal groaning represents less than 1% of
the population consulting at a sleep disorder center.170 However, since this parasomnia is without
major consequences, there is probably a large number of affected individuals
that does not seek medical help. It appears to be three times more prevalent in
men than in women although too few cases have been reported so far to be able
to determine the gender ratio accurately. Onset is habitually during
adolescence or early adulthood and the parasomnia persists for several years.170 The precise time course of the condition is
unknown due to lack of follow-up on this recently identified condition.
Polysomnographic characteristics
Catathrenia occurs during either REM or NREM
sleep but episodes arise predominantly from REM sleep; only one patient
presented groaning exclusively in NREM sleep.170 PSG tracings reveal bradypneic events, often occurring
in clusters, with deep inspirations followed by long expirations and monotonous
vocalization. There is a high night-to-night consistency of the groaning
episodes.171 Although catathrenia is associated with
bradypneic events, only one of the reported cases168 had significant obstructive apneas or
hypopneas and an oxygen saturation remaining above 90% across the night. Body
position does not seem to have any influence.170 Whereas the loud sounds of snoring or
obstructive sleep apneas occur during the inspiratory phase, the vocalizations
of catathrenia occur during expiration. Unlike sleep apnea, sleep architecture
for nocturnal groaners is usually preserved. However, a few patients will show
either reduced total sleep time combined with reduced sleep efficiency, or a
reduction of either slow-wave or REM sleep.170
Associated factors
Neurological and physical (including
otorhinolaryngologic) examination, routine laboratory testing and medical
history show no specific anomaly.170-172 Apart from the fact that a small
proportion of patients (7%) present concomitant bruxism, there are no
associated conditions or obvious predisposing factors.170 As for many parasomnias,
catathrenia seems to be, at least in part, genetically determined. In about 15%
of cases, there is at least one family relative also affected, sometimes in a
way consistent with an autosomal dominant pattern of inheritance.170
1.
American Academy of Sleep Medicine,
Task Force Chair HP: ICSD-II.
International classification of sleep disorders: Diagnostic and coding manual,
Chicago, American Academy of Sleep Medicine, 2005
2. Hillman DR, Murphy AS, Pezzullo L (2006)
The economic cost of sleep disorders. Sleep,
29:299-305.
3. Broughton R, Billings R, Cartwright R,
Doucette D, et al (1994) Homicidal somnambulism: a case report. Sleep, 17:253-264.
4. Kayumov L, Pandi-Perumal SR, Fedoroff P,
Shapiro CM (2000) Diagnostic values of polysomnography in forensic medicine. Journal of Forensic Sciences, 45:191-194.
5. Mahowald MW, Bundlie SR, Hurwitz TD,
Schenck CH (1990) Sleep violence--forensic science implications: polygraphic
and video documentation. Journal of
Forensic Sciences, 35:413-432.
6. Mahowald MW, Schenck CH (2005) Violent
parasomnias: forensic medicine issues, in Principles
and practice of sleep medicine. Edited by Kryger MH, Roth T, Dement WC.
Philadelphia, Elsevier Saunders, pp 960-968.
7. Mahowald MW, Schenck CH, Goldner M,
Bachelder V, et al (2003) Parasomnia pseudo-suicide. J Forensic Sci, 48:1158-1162.
8. Mahowald MW, Schenck CH, Cramer Bornemann
MA (2005) Sleep-related violence. Current
Neurology and Neuroscience Reports, 5:153-158.
9. Oswald I, Evans J (1985) On serious
violence during sleep-walking. Br J Psychiatr,
147:688-691.
10. Rosenfeld DS, Elhajjar AJ (1998) Sleepsex: a variant of
sleepwalking. Archives of Sexual
Behavior, 27:269-278.
11. Schenck CH, Mahowald MW (1995) A polysomnographically
documented case of adult somnambulism with long-distance automobile driving and
frequent nocturnal violence: parasomnia with continuing danger as a noninsane
automatism? Sleep, 18:765-772.
12. Shapiro CM, Trajanovic NN, Fedoroff JP (2003) Sexsomnia--a new
parasomnia? Can J Psychiatr, 48:311-317.
13. Cartwright R (2000) Sleep-related violence: does the
polysomnogram help establish the diagnosis? Sleep
Med, 1:331-335.
14. Schenck CH, Hurwitz TD, Mahowald MW (1993) Normal and abnormal
REM sleep regulation: REM sleep behaviour disorder: an update on a series of 96
patients and a review of the world literature. J Sleep Res, 2:224-231.
15. Olson EJ, Boeve BF, Silber MH (2000) Rapid eye movement sleep
behaviour disorder: demographic, clinical and laboratory findings in 93 cases. Brain, 123:331-339.
16. Yeh SB, Schenck CH (2004) A case of marital discord and
secondary depression with attempted suicide resulting from REM sleep behavior
disorder in a 35-year-old woman. Sleep
Med, 5:151-154.
17. Iranzo A, Molinuevo JL, Santamaria J, Serradell M, et al
(2006) Rapid-eye-movement sleep behaviour disorder as an early marker for a
neurodegenerative disorder: a descriptive study. Lancet Neurology, 5:572-577.
18. Schenck CH, Bundlie SR, Mahowald MW. REM behavior disorder
(RBD): delayed emergence of parkinsonism and/or dementia in 65% of older men
initially diagnosed with idiopathic RBD, and an analysis of the minimum &
maximum tonic and/or phasic electromyographic abnormalities found during REM
sleep. Sleep. 2003;26:A316[Abstract]
19. Nielsen T, Paquette T (2007) Dream-associated behaviors
affecting pregnant and postpartum women. Sleep,
30:1162-1169.
20. Belicki D, Belicki K (1982) Nightmares in a university
population. Sleep Res, 11:116.
21. Bixler EO, Kales A, Soldatos CR, Kales JD, et al (1979)
Prevalence of sleep disorders in the Los Angeles metropolitan area. Am J Psychiatr, 136:1257-1262.
22. Haynes SN, Mooney DK (1975) Nightmares: etiological,
theoretical, and behavioral treatment considerations. Psychol Rec, 25:225-236.
23. Ohayon MM, Morselli PL, Guilleminault C (1997) Prevalence of
nightmares and their relationship to psychopathology and daytime functioning in
insomnia subjects. Sleep, 20:340-348.
24. Simard V, Nielsen TA, Tremblay RE, Boivin M, et al (2008)
Longitudinal study of bad dreams in preschool children: prevalence, demographic
correlates, risk and protective factors. Sleep,
31:62-70.
25. Nielsen TA, Levin R (2005) Nightmare frequency by age, gender
and 9/11: findings from an internet questionnaire. Sleep, 28 (Abstract Supplement):A52.
26. Nielsen TA, Laberge L, Tremblay R, Vitaro F, et al (2000)
Development of disturbing dreams during adolescence and their relationship to
anxiety symptoms. Sleep, 23:727-736.
27. Schredl M, Pallmer R (1998) Geschlechtsspezifische
Unterschiede in Angsttraumen von Schulerinnen und Schulern [Gender differences
in anxiety dreams of school-aged children]. Praxis
der Kinderpsychologie und Kinderpsychiatrie, 47:463-476.
28. Fisher C, Byrne J, Edwards A, Kahn E (1970) A
psychophysiological study of nightmares. J
Am Psychoanal Assoc, 18:747-782.
29. Germain A, Nielsen TA (2003) Sleep pathophysiology in PTSD and
idiopathic nightmare sufferers. Biol
Psychiatry, 54:1092-1098.
30. Woodward SH, Arsenault NJ, Murray C, Bliwise DL (2000)
Laboratory sleep correlates of nightmare complaint in PTSD inpatients. Biol Psychiatry, 48:1081-1087.
31. Harvey AG, Jones C, Schmidt DA (2003) Sleep and posttraumatic
stress disorder: a review. Clin Psychol
Rev, 23:377-407.
32. Orr SP, Roth WT (2000) Psychophysiological assessment:
clinical applications for PTSD. J Affect
Disord, 61:225-240.
33. Pitman RK, Orr SP, Shalev AY, Metzger LJ, et al (1999)
Psychophysiological alterations in post-traumatic stress disorder. Seminars in Clinical Neuropsychiatry, 4:234-241.
34. Woodward SH, Leskin GA, Sheikh JI (2003) Sleep respiratory
concomitants of comorbid panic and nightmare complaint in post-traumatic stress
disorder. Depress Anxiety, 18:198-204.
35. Hublin C, Kaprio J, Partinen M, Koskenvuo M (1999) Nightmares:
Familial aggregation and association with psychiatric disorders in a nationwide
twin cohort. Am J Med Genet, 88:329-336.
36. Kales A, Soldatos CR, Caldwell AB, Charney DS, et al (1980)
Nightmares: clinical characteristics and personality patterns. Am J Psychiatr, 137:1197-1201.
37. Zadra A, Donderi DC (2000) Nightmares and bad dreams: their
prevalence and relationship to well-being. J
Abn Psychol, 109:273-281.
38. Kramer M, Schoen LS, Kinney L (1984) Psychological and
behavioral features of disturbed dreamers. Psychiatr
J U Ottawa, 9:102-106.
39. Starker S (1984) Daydreams, nightmares, and insomnia: The
relation of waking fantasy to sleep disturbances. Imagination, Cognition and Personality, 4:237-248.
40. Cowen D, Levin R (1995) The use of the Hartmann boundary
questionnaire with an adolescent population. Dreaming, 5:105-114.
41. Hartmann E, Elkin R, Garg M (1991) Personality and dreaming:
the dreams of people with very thick or very thin boundaries. Dreaming, 1:311-324.
42. Schredl M, Schafer G, Hofmann F, Jacob S (1999) Dream content
and personality: thick vs. thin boundaries. Dreaming,
9:257-263.
43. Pietrowsky R, Köthe M (2003) Personal boundaries and
nightmare consequences. Dreaming, 13:245-254.
44. Tanskanen A, Tuomilehto J, Viinamaki H, Vartiainen E, et al
(2001) Nightmares as predictors of suicide. Sleep,
24:845-848.
45. Levin R, Nielsen TA (2007) Disturbed dreaming, posttraumatic
stress disorder, and affect distress: a review and neurocognitive model. Psychol Bull, 133:482-528.
46. Nielsen T, Levin R (2007) Nightmares: A new neurocognitive
model. Sleep Med Rev, 11:295-310.
47. Barrett D: Trauma and
dreams, Cambridge, Massachusetts, Harvard University Press, 1996
48. Husni M, Cernovsky ZZ, Koye N, Haggarty J (2001) Nightmares of
refugees from Kurdistan. J Nerv Ment Dis,
189:557-558.
49. Cheyne JA, Rueffer SD, Newby-Clark IR (1999) Hypnagogic and
hypnopompic hallucinations during sleep paralysis: neurological and cultural
construction of the night-mare. Conscious
Cogn, 8:319-337.
50. Solomonova E, Nielsen T, Stenstrom P, Simard V, et al (2008)
Sensed presence as a correlate of sleep paralysis distress, social anxiety and
waking state social imagery. Conscious
Cogn, 17:49-63.
51. Cheyne JA (2001) The ominous numinous. Journal of Consciousness Studies, 8:133-150.
52. Ohayon MM, Guilleminault C, Priest RG (1999) Night terrors, sleepwalking, and confusional arousals in the general population: their frequency and relationship to other sleep and mental disorders. J Clin Psychiatr, 60:268-276.
53. Kotorii T, Uchimura N, Hashizume Y, Shirakawa S, et al (2001) Questionnaire relating to sleep paralysis. Psychiatr Clin Neurosci, 55:265-266.
54. Fukuda
K, Miyasita A, Inugami M, Ishihara K (1987) High prevalence of isolated sleep
paralysis: Kanashibari phenomenon in
Japan. Sleep, 10:279-286.
55. Spanos NP, DuBreuil C, McNulty SA, Pires M, et al (1995) The
frequency and correlates of sleep paralysis in a university sample. J Res Pers, 29:285-305.
56. Hufford D (1995) Awakening paralyzed in the presence of a
"strange visitor", in Alien
Discussions: proceedings of the abduction study conference, Massachusetts
Institute of Technology, June 1992. Edited by Pritchard A, Pritchard DE,
Mack JE, Kasey P, Yapp C. Cambridge, MA, North Cambridge Press, pp 348-353.
57. Hishikawa Y, Shimizu T (1995) Physiology of REM sleep,
cataplexy, and sleep paralysis, in Negative
motor phenomena. Advances in neurology, Vol. 67. Edited by Fahn S, Hallett
M, Luders HO, Marsden CD. Philadelphia, Lippincott-Raven, pp 245-271.
58. Takeuchi T, Fukuda K, Sasaki Y, Inugami M, et al (2002)
Factors related to the occurrence of isolated sleep paralysis elicited during a
multi-phasic sleep-wake schedule. Sleep, 25:89-96.
59. Giaquinto S, Pompeiano O, Somogyi I (1964) Supraspinal
modulation of heteronymous monosynaptic and of polysynaptic reflexes during
natural sleep and wakefulness. Archives
Italiennes de Biologie, 102:230-244.
60. Cheyne JA (2005) Sleep paralysis episode frequency and number,
types, and structure of associated hallucinations. J Sleep Res, 14:319-324.
61. Wing YK, Lee ST, Chen CN (1994) Sleep paralysis in Chinese:
Ghost oppression phenomenon in Hong Kong. Sleep,
17:609-613.
62. Arikawa H, Templer DI, Brown R, Cannon W.G., et al (1999) The
structure and correlates of Kanashibari. J
Psychol, 133:369-375.
63. Hinton DE, Pich V, Chhean D, Pollack MH, et al (2005) Sleep
paralysis among Cambodian refugees: association with PTSD diagnosis and
severity. Depress Anxiety, 22:47-51.
64. Yeung A, Xu Y, Chang DF (2005) Prevalence and illness beliefs
of sleep paralysis among Chinese psychiatric patients in China and the United
States. Transcultural Psychiatry, 42:135-145.
65. McNally RJ, Clancy SA (2005) Sleep paralysis, sexual abuse,
and space alien abduction. Transcultural
Psychiatry, 42:113-122.
66. Szklo-Coxe M, Young T, Finn L, Mignot E (2007) Depression:
relationships to sleep paralysis and other sleep disturbances in a community
sample. J Sleep Res, 16:297-312.
67. Alfonso SS (1991) Isolated sleep paralysis in patients with
disorders due to anxiety crisis. Actas
Luso Esp Neurol Psiquiatr Cienc Afines, 19:58-61.
68. Bell CC, Hildreth CJ, Jenkins EJ, Carter C (1988) The
relationship of isolated sleep paralysis and panic disorder to hypertension. Journal of the National Medical Association,
80:289-294.
69. Paradis CM, Friedman S (2005) Sleep paralysis in African
Americans with panic disorder. Transcultural
Psychiatry, 42:123-134.
70. Simard V, Nielsen TA (2005) Sensed presence as a possible
manifestation of social anxiety. Dreaming,
15:245-260.
71. de Jong JT (2005) Cultural variation in the clinical
presentation of sleep paralysis. Transcultural
Psychiatry, 42:78-92.
72. Hufford DJ: The terror
that comes in the night: An experience-centered study of supernatural assault
traditions, Philadelphia, University of Pennsylvania Press, 1982
73. Schenck CH, Bundlie SR, Ettinger MG, Mahowald MW (1986)
Chronic behavioral disorders of human REM sleep: a new category of parasomnia. Sleep, 9:293-308.
74. Schenck CH, Mahowald MW (2002) REM sleep behavior disorder:
clinical, developmental, and neuroscience perspectives 16 years after its
formal identification in SLEEP. Sleep, 25:120-138.
75. Mahowald MW, Schenck CH (2005) REM sleep parasomnias, in Principles and practice of sleep medicine.
Edited by Kryger MH, Roth T, Dement WC. Philadelphia, Elsevier Saunders, pp
897-916.
76. Nielsen TA (2005) Disturbed dreaming in medical conditions, in
Principles and practice of sleep medicine.
Edited by Kryger M, Roth N, Dement WC. Philadelphia, Elsevier Saunders, pp
936-945.
77. Fantini ML, Corona A, Clerici S, Ferini-Strambi L (2005)
Aggressive dream content without daytime aggressiveness in REM sleep behavior
disorder. Neurology, 65:1010-1015.
78. Ohayon MM, Caulet M, Priest RG (1997) Violent behavior during
sleep. J Clin Psychiatr, 58:369-376.
79. Chiu HF, Wing YK, Lam LC, Li SW, et al (2000) Sleep-related injury
in the elderly - an epidemiological study in Hong Kong. Sleep, 15:513-517.
80. Nielsen T, Svob C, Kuiken D (2009) Dream-enacting behaviors in
a normal population. Sleep, (in
press)
81. Massicotte-Marquez J, Carrier J, Decary A, Mathieu A, et al (2005)
Slow-wave sleep and delta power in rapid eye movement sleep behavior disorder. Annals of Neurology, 57:277-282.
82. Fantini ML, Gagnon JF, Petit D, Rompre PH, et al (2003)
Slowing of electroencephalogram in rapid eye movement sleep behavior disorder. Annals of Neurology, 53:774-780.
83. Boeve BF, Silber MH, Ferman TJ, Lucas JA, et al (2001)
Association of REM sleep behavior disorder and neurodegenerative disease may
reflect an underlying synucleinopathy. Mov
Dis, 16:622-630.
84. Comella CL, Nardine TM, Diederich NJ, Stebbins GT (1998)
Sleep-related violence, injury, and REM sleep behavior disorder in Parkinson's
disease. Neurology, 51:526-529.
85. Gagnon JF, Bedard MA, Fantini ML, Petit D, et al (2002) REM
sleep behavior disorder and REM sleep without atonia in Parkinson's disease. Neurology, 59:585-589.
86. Schenck CH, Bundlie SR, Mahowald MW (1996) Delayed emergence
of a parkinsonian disorder in 38% of 29 older men initially diagnosed with
idiopathic rapid eye movement sleep behaviour disorder. Neurology, 46:388-393.
87. Boeve BF, Silber MH, Ferman TJ, Kokmen E, et al (1998) REM
sleep behavior disorder and degenerative dementia: an association likely
reflecting Lewy body disease. Neurology, 51:363-370.
88. Ferman TJ, Boeve BF, Smith GE, Silber MH, et al (1999) REM
sleep behavior disorder and dementia: cognitive differences when compared with
AD. Neurology, 52:951-957.
89. Plazzi G, Corsini R, Provini F, Pierangeli G, et al (1997) REM
sleep behavior disorders in multiple system atrophy. Neurology, 48:1094-1097.
90. Tachibana N, Kimura K, Kitajima K, Shinde A, et al (1997) REM
sleep motor dysfunction in multiple system atrophy: with special emphasis on
sleep talk as its early clinical manifestation. J Neurol Neurosurg Psychiatr, 63:678-681.
91. Wetter TC, Collado-Seidel V, Pollmacher T, Yassouridis A, et
al (2000) Sleep and periodic leg movement patterns in drug-free patients with
Parkinson's disease and multiple system atrophy. Sleep, 23:361-367.
92. Gagnon JF, Petit D, Fantini ML, Rompré S, et al (2006)
REM sleep behavior disorder and REM sleep without atonia in probable Alzheimer
disease. Sleep, 29:1309-1313.
93. Arnulf I, Merino-Andreu M, Bloch F, Konofal E, et al (2005)
REM sleep behavior disorder and REM sleep without atonia in patients with
progressive supranuclear palsy. Sleep, 28:349-354.
94. Caselli RJ, Chen K, Bandy D, Smilovici O, et al (2006) A
preliminary fluorodeoxyglucose positron emission tomography study in healthy
adults reporting dream-enactment behavior. Sleep,
29:927-933.
95. Postuma RB, Lang AE, Massicotte-Marquez J, Montplaisir J
(2006) Potential early markers of Parkinson disease in idiopathic REM sleep
behavior disorder. Neurology, 66:845-851.
96. Fantini ML, Michaud M, Gosselin N, Lavigne G, et al (2002)
Periodic leg movements in REM sleep behavior disorder and related autonomic and
EEG activation. Neurology, 59:1889-1894.
97. Ferini-Strambi L, Zucconi M (2000) REM sleep behavior
disorder. Clin Neurophysiol, 111
Suppl 2:S136-S140.
98. Fantini ML, Ferini-Strambi L, Montplaisir J (2005) Idiopathic
REM sleep behavior disorder: toward a better nosologic definition. Neurology, 64:780-786.
99. Ferini-Strambi L, Di Gioia MR, Castronovo V, Oldani A, et al
(2004) Neuropsychological assessment in idiopathic REM sleep behavior disorder
(RBD): does the idiopathic form of RBD really exist? Neurology, 62:41-45.
100. Rosen
G, Mahowald MW, Ferber R (1995) Sleepwalking, confusional arousals, and sleep
terrors in the child, in Principles and
practice of sleep medicine in the child. Edited by Ferber R, Kryger M.
Philadelphia, WB Saunders Company, pp 99-106.
101. Ohayon
MM, Priest RG, Zulley J, Smirne S (2000) The place of confusional arousals in
sleep and mental disorders: findings in a general population sample of 13,057
subjects. J Nerv Ment Dis, 188:340-348.
102. Masand
P (1995) Sleepwalking. Am Fam Phys, 51:649-653.
103. Howard
C, D'Orban P (1987) Violence in sleep: medico-legal issues and two case
reports. Psychol Méd, 17:915-925.
104. Ovuga
EBL (1992) Murder during sleep-walking. East
African Medical Journal, 69:533-534.
105. Hartmann
E (1983) Two case reports: night terrors with sleepwalking -- a potentially
lethal disorder. J Nerv Ment Dis, 171:503-505.
106. Gottlieb
P, Christensen O, Kramp P (1986) On serious violence during sleepwalking. Br J Psychiatr, 149:120-121.
107. Klackenberg
G (1982) Somnambulism in childhood - prevalence, course and behavioral
correlations: a prospective longitudinal study (6-16 years). Acta Paediatrica Scandinavica, 71:495-499.
108. Laberge
L, Tremblay RE, Vitaro F, Montplaisir J (2000) Development of parasomnias from
childhood to early adolescence. Pediatrics,
106:67-74.
109. Shang
CY, Gau SS, Soong WT (2006) Association between childhood sleep problems and
perinatal factors, parental mental distress and behavioral problems. J Sleep Res, 15:63-73.
110. Petit
D, Touchette E, Tremblay RE, Boivin M, et al (2007) Dyssomnias and parasomnias
in early childhood. Pediatrics, 119:e1016-e1025.
111. Blatt
I, Peled R, Gadoth N, Lavie P (1991) The value of sleep recording in evaluating
somnambulism in young adults. Electroencephalogr
Clin Neurophysiol, 78:407-412.
112. Denesle
R, Nicolas A, Gosselin A, Zadra A, et al (1998) Sleepwalking and aggressive
behavior in sleep. Sleep, 21
(suppl.1):70.
113. Gaudreau
H, Joncas S, Zadra A, Montplaisir J (2000) Dynamics of slow-wave activity
during the NREM sleep of sleepwalkers and control subjects. Sleep, 23:755-760.
114. Guilleminault
C, Leger D, Philip P, Ohayon MM (1998) Nocturnal wandering and violence: review
of a sleep clinic population. Journal of
Forensic Sciences, 43:158-163.
115. Schenck
CH, Milner DM, Hurwitz TD, Bundlie SR, et al (1989) A polysomnographic and
clinical report on sleep-related injury in 100 adult patients. Am J Psychiatr, 146:1166-1173.
116. Schenck
CH, Pareja JA, Patterson AL, Mahowald MW (1998) Analysis of polysomnographic
events surrounding 252 slow-wave sleep arousals in thirty-eight adults with
injurious sleepwalking and sleep terrors. J
Clin Neurophysiol, 15:159-166.
117. Joncas
S, Zadra A, Paquet J, Montplaisir J (2002) The value of sleep deprivation as a
diagnostic tool in adult sleepwalkers. Neurology,
58:936-940.
118. Pilon
M, Zadra A, Joncas S, Montplaisir J (2006) Hypersynchronous delta waves and
somnambulism: brain topography and effect of sleep deprivation. Sleep, 29:77-84.
119. Hublin
C, Kaprio J, Heikkila K, Koskenvuo M (1997) Prevalence and genetic of
sleepwalking: A population-based twin study. Neurology, 48:177-181.
120. Lecendreux
M, Bassetti C, Dauvilliers Y, Mayer G, et al (2003) HLA and genetic
susceptibility to sleepwalking. Mol
Psychiatry, 8:114-117.
121. Cirignotta
F, Zucconi M, Mondini S, Lenzi PL, et al (1983) Enuresis, sleepwalking, and
nightmares: an epidemiological survey in the republic of San Marino, in Sleep/Wake disorder: Natural history,
epidemiology, and long-term evolution. Edited by Guilleminault C, Lugaresi
E. New York, Raven Press, pp 237-241.
122. Crisp
AH, Matthews BM, Oakey M, Crutchfield M (1990) Sleepwalking, night terrors, and
consciousness. Br Med J, 300:360-362.
123. Fisher
C, Kahn E, Edwards A, Davis DM (1973) A psychophysiological study of nightmares
and night terrors: I. Physiological aspects of the Stage 4 night terror. J Nerv Ment Dis, 157:75-98.
124. Fisher
BE, Pauley C, McGuire K (1989) Children's Sleep Behavior Scale: normative data
on 870 children in grades 1 to 6. Percept
Mot Skills, 68:227-236.
125. Simonds
JF, Parraga H (1982) The parasomnias: Prevalence and relationships to each
other and to positive family histories. Hillside
Journal of Clinical Psychiatry, 4:25-38.
126. Vela-Bueno
A, Bixler EO, Dobladez-Blanco B, Rubio ME, et al (1985) Prevalence of night
terrors and nightmares in elementary school children: a pilot study. Res Commun Psychol Psychiatr Behav, 10:177-188.
127. Abe
K, Oda N, Ikenaga K, Yamada T (1993) Twin study on night terrors, fears and
some physiological and behavioral characteristics in childhood. Psychiatric Genetics, 3:39-43.
128. Abe
K, Amatomi M, Oda N (1984) Sleepwalking and recurrent sleeptalking in children
of childhood sleepwalkers. Am J
Psychiatr, 141:800-801.
129. Fergusson
DM, Hons BA, Horwood LJ, Shannon FT (1986) Factors related to the age of
attainment of nocturnal bladder control: an 8-year longitudinal study. Pediatrics, 78:884-890.
130. Byrd
RS, Weitzman M, Lanphear NE, Auinger P (1996) Bed-wetting in US children:
epidemiology and related behavior problems. Pediatrics,
98:414-419.
131. Burgio
KL, Locher JL, Ives DG, Hardin JM, et al (1996) Nocturnal enuresis in
community-dwelling older adults. Journal
of the American Geriatric Society, 44:139-143.
132. Bader
G, Neveus T, Kruse S, Sillen U (2002) Sleep of primary enuretic children and controls.
Sleep, 25:579-583.
133. Wolfish
NM, Pivik RT, Busby KA (1997) Elevated sleep arousal thresholds in enuretic
boys: clinical implications. Acta
Paediatrica, 86:381-384.
134. Touchette
E, Petit D, Paquet J, Tremblay RE, et al (2005) Bedwetting and its association
with developmental milestones in early childhood. Arch Pediatr Adolesc Med, 159:1129-1134.
135. van
Hoecke E, Hoebeke P, Braet C, Walle JV (2004) An assessment of internalizing
problems in children with enuresis. Journal
of Urology, 171:2580-2583.
136. Verduin
TL, Kendall PC (2003) Differential occurrence of comorbidity within childhood
anxiety disorders. Journal of Clinical
Child and Adolescent Psychology, 32:290-295.
137. Fergusson
DM, Horwood LJ (1994) Nocturnal enuresis and behavioral problems in
adolescence: a 15-year longitudinal study. Pediatrics,
94:662-668.
138. von
Gontard A, Schaumburg H, Hollmann E, Eiberg H, et al (2001) The genetics of
enuresis: a review. Journal of Urology, 166:2438-2443.
139. Bakwin
H (1973) The genetics of enuresis, in Bladder
control and enuresis. Edited by Kolvin I, MacKeith RC, Meadow SR. London,
Spastics International Medical Publications, pp 73-77.
140. Lobbezoo
F, Rompre PH, Soucy JP, Iafrancesco C, et al (2001) Lack of associations
between occlusal and cephalometric measures, side imbalance in striatal D2
receptor binding, and sleep-related oromotor activities. Journal of Orofacial Pain, 15:64-71.
141. Lavigne
GJ, Montplaisir JY (1994) Restless legs syndrome and sleep bruxism: prevalence
and association among Canadians. Sleep, 17:739-743.
142. Lavigne
GJ, Manzini C, Kato T (2005) Sleep bruxism, in Principles and practice of sleep medicine. Edited by Kryger MH,
Roth T, Dement WC. Philadelphia, Elsevier Saunders, pp 946-959.
143. Hublin
C, Kaprio J, Partinen M, Koskenvuo M (1998) Sleep bruxism based on self-report
in a nationwide twin cohort. J Sleep Res,
7:61-67.
144. Lavigne
GJ, Rompre PH, Montplaisir JY (1996) Sleep bruxism: validity of clinical
research diagnostic criteria in a controlled polysomnographic study. Journal of Dental Research, 75:546-552.
145. Macaluso
GM, Guerra P, Di Giovanni G, Boselli M, et al (1998) Sleep bruxism is a
disorder related to periodic arousals during sleep. Journal of Dental Research, 77:565-573.
146. Kato
T, Rompre P, Montplaisir JY, Sessle BJ, et al (2001) Sleep bruxism: an oromotor
activity secondary to micro-arousal. Journal
of Dental Research, 80:1940-1944.
147. Huynh
N, Kato T, Rompre PH, Okura K, et al (2006) Sleep bruxism is associated to
micro-arousals and an increase in cardiac sympathetic activity. J Sleep Res, 15:339-346.
148. Manfredini
D, Landi N, Fantoni F, Segu M, et al (2005) Anxiety symptoms in clinically
diagnosed bruxers. Journal of Oral
Rehabilitation, 32:584-588.
149. Casanova-Rosado
JF, Medina-Solis CE, Vallejos-Sanchez AA, Casanova-Rosado AJ, et al (2006)
Prevalence and associated factors for temporomandibular disorders in a group of
Mexican adolescents and youth adults. Clinical
Oral Investigations, 10:42-49.
150. Lavigne
GJ, Lobbezoo F, Rompré PH, Nielsen TA, et al (1997) Cigarette smoking as
a risk factor or an exacerbating factor for restless legs syndrome and sleep
bruxism. Sleep, 20:290-293.
151. Stepanova
I, Nevsimalova S, Hanosova J (2005) Rhythmic movement disorder in sleep
persisting into childhood and adulthood. Sleep,
28:851-857.
152. de
Lissovoy V (1962) Headbanging in early childhood. Child Dev, 33:43-56.
153. Mackenzie
JM (1991) "Headbanging" and fatal subdural haemorrhage. Lancet, 338:1457-1458.
154. Noel
LP, Clarke WN (1982) Self-inflicted ocular injuries in children. American Journal of Ophtalmology, 94:630-633.
155. Spalter
HF, Bemporad JR, Sours JA (1970) Cataracts following chronic headbanging. Archives of Ophtalmology, 83:182-186.
156. Klackenberg
G (1971) A prospective longitudinal study of children. Data on psychic health
and development up to 8 years of age. Acta
Paediatrica Scandinavica Suppl, 224:1-239.
157. Thorpy
MJ (1987) Rhythmical body movements during sleep, in Body movements during sleep. Edited by Segawa M. Tokyo, Sanposha,
pp 47-52.
158. Walters
AS, Hening WA, Chokroverty S (1988) Frequent occurrence of myoclonus while
awake and at rest, body rocking and marching in place in a subpopulation of
patients with restless legs syndrome. Acta
Neurologica Scandinavica, 77:418-421.
159. Chisholm
T, Morehouse RL (1996) Adult headbanging: sleep studies and treatment. Sleep, 19:343-346.
160. Mayer
G, Tracik F, Wilde J (2000) Rhythmic movement disorder revisited. J Sleep Res, 9:127.
161. Arkin
AM, Toth MF, Baker J, Hastey JM (1970) The frequency of sleep talking in the
laboratory among chronic sleep talkers and good dream recallers. J Nerv Ment Dis, 151:369-374.
162. Arkin
AM: Sleep-talking: Psychology and
psychophysiology, Hillsdale, New Jersey, Lawrence Erlbaum, 1981
163. Tani
K, Yoshu N, Yoshino I, Kobayashi E (1966) Electroencephalographic study of
parasomnia: sleep-talking, enuresis and bruxism. Physiol Behav, 1:241-243.
164. Arkin
AM, Toth MF, Baker J, Hastey JM (1970) The degree of concordance between the
content of sleep talking and mentation recalled in wakefulness. J Nerv Ment Dis, 151:373-393.
165. Hublin
C, Kaprio J, Partinen M, Koskenvuo M (1998) Sleeptalking in twins: epidemiology
and psychiatric comorbidity. Behavior
Genetics, 28:289-298.
166. Brunner
DP, Gonzalez HL (2004) Catathrenia: a rare parasomnia with prolonged groaning
during clusters of central or mixed apneas. J
Sleep Res, 13:107.
167. DeRoek
J, VanHoof E, Cluydts R (1983) Sleep-related expiratory groaning. A case
report. Sleep Res, 12:237.
168. Grigg-Damberger
M, Brown LK, Casey KR (2006) A cry in the night: nocturnal moaning in a
12-year-old boy. Journal of Clinical
Sleep Medicine, 2:354-357.
169. Iriarte
J, Alegre M, Urrestarazu E, Viteri C, et al (2006) Continuous positive pressure
as treatment of catathrenia (nocturnal groaning). Neurology, 66:609.
170. Oldani
A, Manconi M, Zucconi M, Castronovo V, et al (2005) 'Nocturnal groaning': just
a sound or parasomnia? J Sleep Res, 14:305-310.
171. Pevernagie
DA, Boon PA, Mariman AN, Verhaeghen DB, et al (2001) Vocalization during
episodes of prolonged expiration: a parasomnia related to REM sleep. Sleep Med, 2:19-30.
172. Vetrugno
R, Provini F, Plazzi G, Vignatelli L, et al (2001) Catathrenia (nocturnal
groaning): a new type of parasomnia. Neurology,
56:681-683.
173. Guilleminault
C, Hagen CC, Khaja AM (2008) Catathrenia: parasomnia or uncommon feature of
sleep disordered breathing? Sleep, 31:132-139.
174. Vetrugno
R, Lugaresi E, Plazzi G, Provini F, et al (2007) Catathrenia (nocturnal
groaning): an abnormal respiratory pattern during sleep. European Journal of Neurology, 14:1236-1243.
175. Siddiqui
F, Walters AS, Chokroverty S (2007) Catathrenia: A rare parasomnia which may
mimic central sleep apnea on polysomnogram. Sleep
Med, 9:460-461.
176. Steinig
J, Lanz M, Krugel R, Happe S (2007) Breath holding - A rapid eye movement (REM)
sleep parasomnia (catathrenia or expiratory groaning). Sleep Med, 9:455-456.